abs medical billing and coding
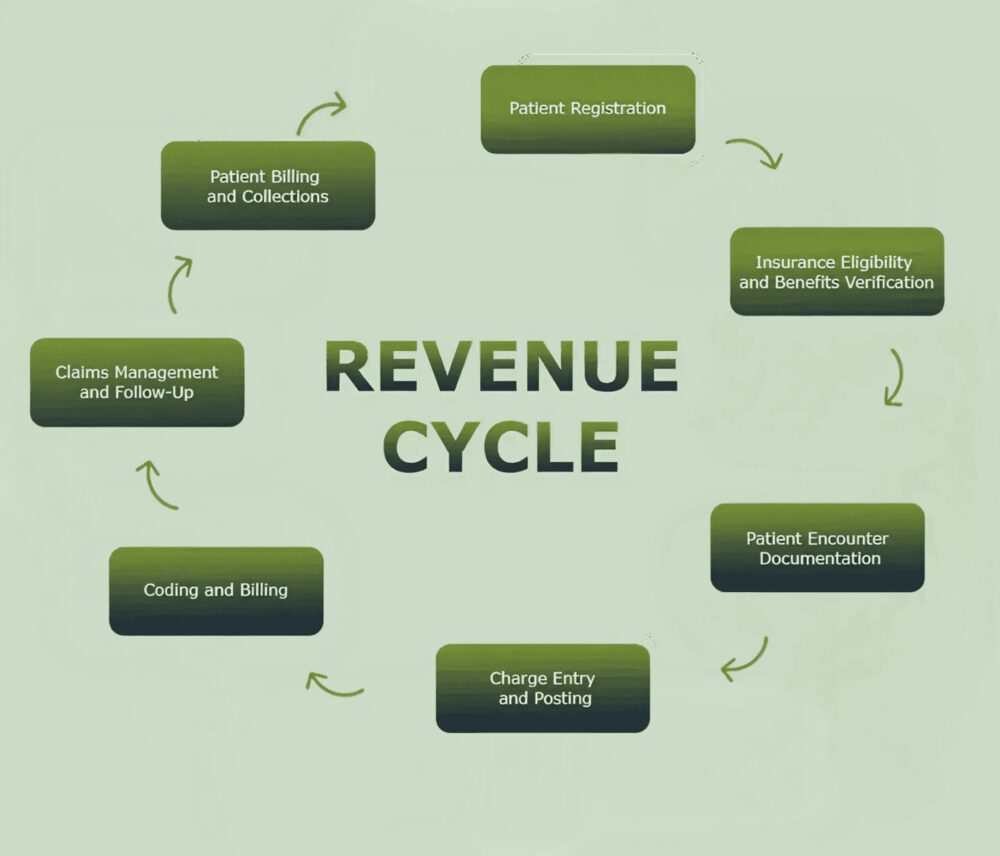
Understanding the healthcare revenue cycle is essential for maintaining accurate billing, timely reimbursement, and compliant operations. Each step is interconnected, and breakdowns at any point can lead to delays, denials, or lost revenue.
ABS Medical Billing and Coding presents structured tutoring that walks practices, staff, and individuals through every stage of the revenue cycle. Our approach focuses on clarity, accuracy, and real-world application so teams understand not only what to do, but why each step matters.
We also offer tutoring for those pursuing CPC (Certified Professional Coder), and CPB (Certified Professional Biller) certifications.

We train staff on efficient registration workflows. This includes proper data collection, such as copying of front and back of insurance card, current and updated demographics, insurance guarantor, and the importance of collecting all co-pays and outstanding balances.

Our tutoring focuses on verifying active coverage, identifying secondary or missing insurance, and communicating benefits accurately. We also guide staff on explaining patient responsibility clearly and professionally to support earlier and more reliable payments.

During the patient visit, services provided must be documented accurately and completely. This documentation drives coding, billing, and compliance.
We help providers and staff understand documentation requirements, regulatory considerations, and communication best practices. Proper encounter documentation reduces coding errors and supports clean claim submission.

Our tutoring focuses on charge capture accuracy, documentation review, and reconciliation processes. Proper charge posting ensures claims reflect the services delivered and supports correct reimbursement amounts.

Medical coding translates clinical documentation into standardized codes required for billing. Errors at this stage often result in denials or underpayments.
We provide guidance on the correct use of diagnosis and procedure codes, payer requirements, and common coding errors. Training emphasizes submitting clean claims the first time to improve cash flow and reduce accounts receivable.

We train teams to review rejected claims, explanations of benefits, identify denial reasons, follow up on unpaid claims, and determine when appeals are appropriate.

We guide practices on clear patient statements, payment workflows, and appropriate collection strategies. A respectful and organized billing process supports patient trust while completing the revenue cycle efficiently.
Customize Your Training
"*" indicates required fields
